Last updated on November 25th, 2023 at 01:54 pm
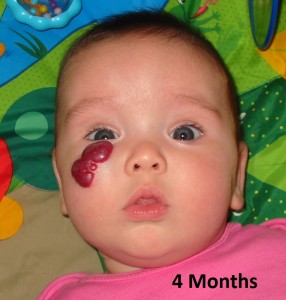
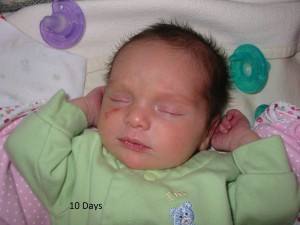
A hemangioma is a type of vascular birthmark. It is estimated that approximately 10% of births have a vascular birthmark. A hemangioma is the most common benign tumor of infancy. Girls are affected 5x more than boys. Light skinned people are affected more often than those of darker complexion. (www.hemangiomatreatment.org). They are also more common in twins. In over 80% of cases they occur on the face or head and neck. Most are not present at birth and become apparent within the first month of life.
The current thought is that hemangiomas develop from cells that cross from the placenta into the baby, become lodged, and grow. There are 2 types of hemangioma, focal and segmental.
Focal hemangiomas are more localized and grow in a tumor like fashion for up to 6 to 9 months. Segmental hemangiomas are more diffuse and flat. These hemangiomas can be very aggressive and locally destructive. This type of hemangioma can proliferate for up to 24 months and can be quite destructive, distorting local tissue contours and ulcerating sometimes with significant tissue loss. Eventually all hemangiomas stop growing and begin to involute (shrink). Each hemangioma will do this at its own pace. Some involute rapidly (over 2 to 3 years) whereas others may take up to 12 years to involute. The end point of involution can be quite variable. Some will involute and leave barely a trace, whereas others will hardly shrink at all. By about 2 to 3 years of age, it should be possible to determine whether or not your child’s hemangioma is shrinking rapidly or not. (www.vbiny.org)
There are several options for treatment. There is no reason in this day and age to accept that the only option is to ‘leave it alone’; and wait for the hemangioma to ‘go away’. While all hemangiomas eventually involute, the result is not always cosmetically acceptable (www.birthmark.org). The most appropriate treatment plan needs to be individualized for each patient and each lesion.
There Are 4 Different Options for Treatment That Can Be Used Singly or in Combination
1. Observation
Sometimes it is appropriate to wait and see what happens.
2. Steroids
Can be used to slow down the growth of the lesion but are only useful during proliferation. The window of opportunity to begin steroid treatment is often very small. The rare lesions that are life threatening are always treated with steroids. Treating an involuting hemangioma with steroids is not useful.
3. Lasers
Treatments with lasers can be used with the goal of completely removing the lesion. There are various laser treatment options available.
4. Surgery
Along with lasers, surgery achieves high results in most patients. There are many misconceptions about operating on hemangiomas one of which is the risk of hemorrhage and www.hemangiomatreatment.org is working to educate physicians.
If your child has multiple hemangiomas, an ultrasound should be done on the entire body to rule out internal lesions.
If you are researching hemangiomas you will likely also find mention of the psycho-social effects that can be a result of a child having to live with a hemangioma. When your child becomes more self-aware between 2 and 3 years old, they will become aware of differences in their appearance from that of other children and their twin.
If your child is diagnosed with a hemangioma or you suspect that your child has a hemangioma be prepared to aggressively advocate for them. The first several weeks are crucial in the case of a hemangioma that is growing aggressively or in a location where it can cause difficulty with breathing or vision.
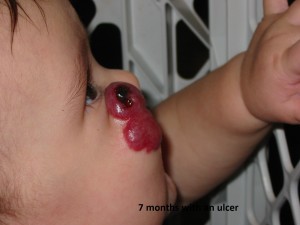
On a personal note, I found the vascular birthmarks foundation (www.birthmark.org) was a great resource for research and support when I was dealing with my daughter’s diagnosis. Her pediatrician advocated for a ‘wait and see’ approach and said that it was really a ‘cosmetic’ issue. For the most part, that has been true. However, when the hemangioma developed an ulcer (at about 7 month) we pushed for referrals to dermatology to try and prevent any long term damage (scarring).

After consultation with dermatology, pediatric dermatology, a visit with a pediatric oncologist and a pediatric ophthalmologist we opted for the wait and see (observation) approach since her vision was not being affected. I believe we made the right choice for her case and our family. I will say that initially, the psycho-social affects were my issue not hers. Not only did I get all the usual twin comments and attention but they were followed by “What’s wrong with her face” or “Did she fall down?”
It was extremely difficult as a new Mom to deal with the negative attention while trying to behave as if it were no big deal so that my daughter would not be negatively impacted. I cannot tell you the number of times I have had to explain to strangers in front of her! As a result, at 3 years old, she had mastered saying hemangioma so when other kids asked what was on her face she would say “It’s my hemangioma” which usually results in the other child losing interest because they have no idea what she is talking about!
Now, she almost has a sense of pride that she has a hemangioma and her identical sister does not. I hope that our decision will continue to be the right one but am open to changing our course should she ever complain about the attention she receives from other children or curious adults.
Written by Charissa Lewis, contributing writer and mama of twins +1.