Last updated on September 30th, 2021 at 10:14 am
Whether you choose to breast feed, pump and bottle feed, or formula feed, one of the first and best ways to bond with your newborn is through the feeding process. You get all cuddly very frequently, at some very intimate times of the day (you know… 3 am), and feel very accomplished and fulfilled as a mother providing a basic necessity for your child. You and your baby are in the perfect position for face to face interactions, and many women report this is the most memorable time they have with their newborn. New parents prepare for baby’s arrival by registering for and buying the newest, latest and greatest bottle, and a myriad of nipples to use. But what happens when infant feeding is not the dream we envisioned it would be? Instead of quiet nights, they are restless nights filled with crying, no sweet cuddles, and the feeling that you as a parent are failing. Your house becomes a battlefield filled with every nipple you have and 12 more styles of bottle than the latest, greatest bottle you started out with. If this was you, because it was me times two with my twins, you are not alone, and you are not a failure. Let’s look at some basics to infant feeding and what to do when things might go wrong.
Throughout this article, three major areas that can affect infant feeding will be discussed along with suggestions if you find yourself in one of those scenarios. I myself dealt with both of my twins having severe reflux as infants, and feeding continues to be an ever-present difficulty in our lives. No one ever plans to experience any extreme issue with their newborn, so it’s nice to realize you are not alone if this occurs, and I strongly suggest seeking out support from those that have experience with these issues.
Overview of Bottles and Nipples

Let’s start with a basic overview of bottles and nipples. It is impossible to know what style of bottle your baby will latch onto and use until they are born and actually using said bottle. What is more important to consider is the type of nipple and to realize there are many styles and levels of flow for nipples. Bottle nipples are generally labeled using an age range in months, which correlates to the time frame it would be appropriate to use with an infant. Most bottle nipple stages run in preemie, newborn, 3-6 months, and 6 + months. The idea behind this is that a nipple for an older infant has a faster flow rate of liquid since older babies are eating more volume at a faster rate.
You may also notice that the nipples for younger babies are firmer to help a baby achieve good suction in order to feed well while learning and getting stronger through the process of feeding from a bottle. In some situations, the equipment used for feeding (namely the breast, bottle, and nipple) make a huge difference in how well feeding goes. One of the most common complaints is that a child is ‘not interested’ in eating, meaning they frequently refuse to eat and turn away. Some parents think they should increase the flow of liquid to help, when, in actuality, this can make feeding worse.
Premature Babies
Having premature babies presents its own unique set of problems when it comes to feeding. Many of the systems needed for adequate feeding are not fully developed, including the respiratory and gastrointestinal systems coupled with weak muscles in and around the mouth.

The first problem that can arise is that preemies are usually delayed feedings by mouth when they are first born due to their medical condition, how early they were born, and how medically stable they become. This delays the bonding process, whether bottle or breast feeding, until the child is stable enough to try this and even then, they may not be able to feed well due to any number of complications. Because preemies do not have fully developed systems at birth, they have trouble coordinating suck-swallow-breathe, the pattern to be able to effectively drink milk, swallow the milk, and breathe. This is usually reflexive, meaning it happens without even thinking about it, in babies born at term.
Preemies may also present decreased endurance to complete feeding and often tire before being able to drink a sufficient amount of milk. Preemies may also have weaker oral motor skills which will make feeding more difficult. Oral motor skills in infants include the ability to use the lips, cheeks, tongue and jaw in coordination to create a suction on a nipple in order to draw a sufficient amount of milk in, and then to use those same body parts to move the milk to the back of the mouth and swallow.
Another major issue that can occur in preemies is reflux. Since the round muscle at the bottom of the esophagus and opening of the stomach, known as the lower esophageal sphincter, is not fully functional until 38 weeks gestation, more than half of preemies will experience reflux. Reflux will be discussed in more detail later in this article. Here are some strategies you may see or use with a premature baby in the NICU:
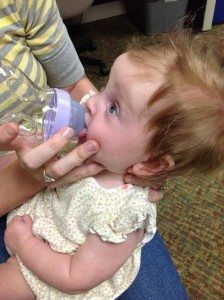
Supplemental Feeding: Many times preemies in the NICU will be given supplemental feedings through an oral-gastric tube (OG tube), a thin tube fed through the infants mouth and into the stomach, or through a naso-gastric tube (NG tube), a thin tube fed through the infants nose and into the stomach. These tube feedings are given after the infant attempts feeding by mouth and ensures that the infant receives the correct volume of milk needed for weight gain in a standard time frame, while the infant learns to eat by mouth and strengthens oral motor skills that may be weak.
If you choose to pump while your baby is in the NICU with the plan of breast feeding once your baby is strong enough to do so, be sure to follow the hospitals guidelines on storing and transporting your colostrum and breast milk to ensure none is wasted. Hospitals often times have stricter guidelines on how long breast milk can be stored before needing to be thrown out for fear of making an infant sick. And nothing makes a mother more angry or upset than her liquid gold being lost or wasted.
If you find yourself in the NICU with your baby and he or she is having trouble feeding, ask for a lactation consultation and/or a screening from an occupational or speech therapist. When in a NICU setting, these professionals are skilled at infant feeding and can offer many simple suggestions.
Babies with Gastroesophageal Reflux

Gastroesophageal reflux (GER) is a very real issue in many infants and often times goes undiagnosed and untreated. GER is difficult to diagnosis in infants and young children due to the fact that the few tests that are available to test for it are somewhat unreliable and often give false negative results. It is normal for babies to spit up and ‘reflux,’ but this becomes a problem when the frequency of these episodes is extremely high, occur multiple times throughout the day and night, and if the episodes occur 30 minutes or later after a feed, as this is a time when the food has become acidified and causes more of a burning sensation in the esophagus. If left untreated, babies can experience feeding issues related well into toddlerhood because they have learned that feeding hurts. If you experienced a burning in your chest and throat every time you ate, you would not want to eat either.
Some general signs and symptoms of reflux in babies include: signs of discomfort like crying or grimacing with feeding, arching of the neck and back, spit up or vomiting, gagging with feeding, preference of spoon feeding over bottle feeding in babies 6 months and older, eating smaller amounts of food more times during the day, great variability in feeding amounts from day to day, poor sleeping habits, poor suck on a bottle or nipple but a strong suck on a pacifier, poor weight gain, and/or resistance to feedings.
Sometimes, if reflux is severe enough in a baby, they will exhibit a subtle reflex known as Sandifer’s reflex. With Sandifer’s reflex, a baby will arch back and turn their head to the right and only to the right. Babies with reflux move into this position to seek comfort from the burning sensation because when they arch back and move their head to the right, they are elongating and closing off part of the esophagus which reduces reflux in the moment. If you notice any of these signs and symptoms with your baby, you should seek out medical guidance from your pediatrician or a specialist known as a pediatric gastroenterologist. If your child is diagnosed with reflux, you should question what may be causing the reflux as different causes can warrant different treatment strategies.
If your child has been diagnosed with reflux and you have consulted with your pediatrician or a specialist, you may have started giving your child some medication or changing their formula or diet to help alleviate the symptoms they were once experiencing. Reflux will typically continue to happen until a child is over 12-18 months of age, but with medication and/or diet changes, they will feel more comfortable and, in turn, feeding can be pleasurable for the entire family again. Here are some other strategies you can try at home to help with reflux symptoms:

Positioning: If breast feeding, change the position of your baby to get them more upright while feeding. Try having baby belly-to-belly with you or in a football hold, but angled to keep them moderately upright and still providing head support. An upright posture helps keep reflux down because you’ve gravity working for you. After feedings, position baby in a swing, bouncy seat or on an inclined couch cushion for 30 minutes. You can change a diaper on an inclined couch cushion if you really need to; if you do, be sure to roll baby side to side to clean and not press their legs into their tummy. An infant car seat is not a good option as an after feeding position as the hips are bent towards the tummy too much and can put pressure on the baby’s tummy making reflux worse. When burping a baby, be sure to position them upright and with their head over your shoulder. DO NOT hold them in your lap and position them forward as this puts pressure on the tummy and can make reflux worse. Try to carry your baby with their belly towards your body and not with their back to your body. The position of your arm when supporting baby is often on the tummy and again provides too much pressure making reflux worse.

Rice Cereal: Sometimes a health professional will recommend adding 1-2 teaspoons of rice cereal to baby’s bottle to make the fluid thicker. This helps keep the fluid in the tummy making it harder to reflux. If this is the case, follow the guidelines set up by your healthcare professional closely.
Dysphagia and Aspiration
Dysphagia is the medical term for difficulty swallowing. With dysphagia, a child can have trouble swallowing safely or may not be able to swallow at all. A negative side effect of dysphagia can be aspiration, which is the movement of fluid or food into the lungs while attempting to swallow. Aspiration can be very scary as it can cause repeat infections of the lungs and, at its worst, can be fatal. With proper treatment and guidance, aspiration can be well managed, and children can learn to safely eat and swallow.
These issues can show up soon after a child is born but sometimes do not manifest until after 6 months old. This occurs because after 6 months of age children are learning to sit more independently and have good head control. As children grow into these more mature postures, the structures in their throats begin to grow and spread apart and it becomes the main job of the epiglottis, a small flap in the back of the throat above the esophagus, to close off the airway and direct food into the esophagus.
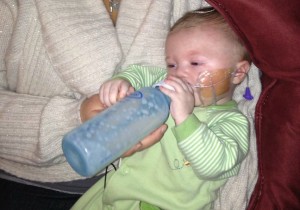
Some warning signs of aspiration and swallowing difficulties include: increased and excessive congestion and coughing, wet sounds with breathing, signs of discomfort with feeding, refusal to eat, choking during feedings, turning blue around the lips while feeding, watering eyes with a red face during feeding, and/or frequent infections like pneumonia. If you suspect that your child may be aspirating, contact your pediatrician immediately. The standard test for swallowing difficulties is a modified barium swallow, which is a live action x-ray to watch where liquids of various thicknesses travel when a child swallows. If your child has been diagnosed with dysphagia or aspiration, a healthcare practitioner will monitor their care closely and most likely will recommended thickening fluids to a certain consistency. It is imperative that you follow these guidelines to ensure your child will swallow safely. In conjunction with thickening liquids, they may recommend oral motor strengthening with an occupational or speech therapist.
Feeding should be an enjoyable experience for all involved, but sometimes unforeseen complications arise and can complicate things. If you believe your child has a feeding problem or is not gaining weight well, contact your pediatrician and begin a dialogue about a referral for a feeding evaluation by an occupational therapist. Hopefully, with the right diagnosis and treatment, feeding can once again be a blissful experience for parents and baby.

Megan Carpenter has been an occupational therapist for 7 years with 5 years of experience in pediatrics at United Cerebral Palsy of Greater Birmingham. Megan is married and is also a mother of 3 year old twin girls who constantly keep her busy but fill her life with much joy. Both of her girls experienced severe reflux as infants, and as a result, Megan has turned her professional focus to pediatric feeding, eating and swallowing. Megan can be contacted at mcarpenter@ucpbham.com with any questions related to the information in this article. Click here to read all of Megan’s articles on Twiniversity.







