Last updated on August 18th, 2023 at 11:58 am
At 39.5 years old and single, I decided it was time to make true on my statement that I would have kids on my own if I hadn’t found the right partner. So I went through invitro-fertilization and thankfully – I was pregnant. I could not have been happier, or more scared that something could go wrong.
An early ultrasound showed that she was perfect – she had 10 perfect fingers and 10 perfect toes, and was seemingly training for the Olympic soccer team. After the doctor pointed out these many perfections, he dropped the bomb: I had a chorioamniotic membrane separation; the layers of the placenta that should have fused by 15 weeks had not done so, and the ramifications could be very serious. He pushed me to do further testing that could harm my daughter, and I refused. His words, “The only way you will know anything for certain is to end the pregnancy,” inspired in me the most violent reaction I have ever felt. I refused to terminate my pregnancy.

The biggest fear of this complication was that she could come very early (and possibly not viable), and come early she did. When I realized that my water was leaking at 26.5 weeks, a tremendous fear clutched my heart – my worst nightmare was coming true. Thankfully, through hospitalized bed rest and very close monitoring, we were able to keep her cooking inside of me for another 3 weeks. All along I was counseled that I should think about what measures I would want taken to save my child if she were born very early. I didn’t need to think about it for a second. “All measures,” I continually said. I was so incredibly attached and tied to her already that I couldn’t imagine not doing everything possible to save her.
One day shy of 30 weeks, she decided she wasn’t waiting anymore. Amazingly, she was quite healthy, just very small. She was thus termed a “feeder and grower” in the NICU, where she would live for the next 2 months. I called her my perfect little mini muffin, because even at 2 pounds, she was a miniature version of perfection. “She’s scrawny, but she’s feisty!” we heard over and over from the nurses. She may have been no bigger than a small cantaloupe, but her spirit was immediately apparent and larger than life.

I spent hours each day in the NICU performing “kangaroo care.“ While a baby so small does not like to be stroked, I was told that holding her skin-to-skin was the best thing I could do for her development at that time. All 10 inches of her only reached from under my chin to my ribs. We spent the time between each of her rest periods in this position. Holli sleeping and me singing or talking to her while anxiously watching the screen monitoring her oxygen and heart rate.
“I knew she was a genius!” I declared the first time she was “old” enough to breastfeed, still in the NICU. I had expected a much bigger hurdle, but she instinctively knew just what to do and went right at it. But the biggest hurdle was yet to come. The next day she developed a terrible infection, starting with a rash that I noticed as I held her. By the following day she was as white as a sheet and not moving. The doctors brought me back to a private room to tell me “Holli is a very sick little girl.” I asked one of them for the worst case scenario. “I don’t want to talk about worst case scenarios with Holli” was the reply. Although the infection was never identified, it did respond to antibiotics and she again fought her way through and came out kicking. Possibly as a result of having been intubated, afterward she was not as interested in breastfeeding or even bottle feeding, and would stay on a feeding tube through the next four years.
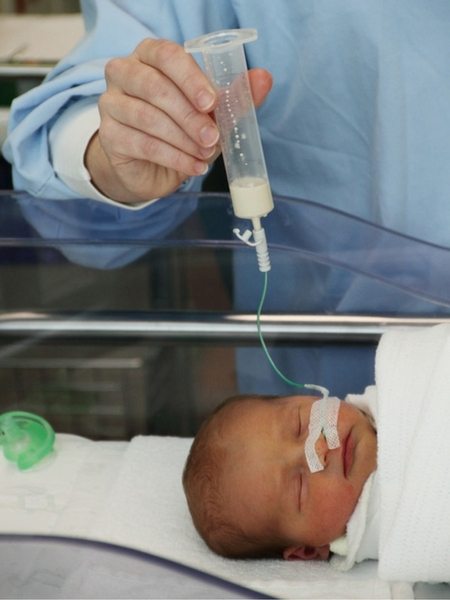
I was continually assured that a “lightbulb” would go off in Holli’s head and she would suddenly put together the sucking-swallowing-breathing connection this is so difficult to learn but somehow comes very naturally to almost every baby. In a continuation of her stubborn nature, Holli continuously decided she would rather not eat. Because she was ready to come home in every other way, at 2 months and 4 pounds, I found myself taking a crash course in administering food through a feeding tube and reinserting the tube through her nose into her stomach each time she either managed to pull it out or threw it up in the midst of one of her violent reflux attacks.
What was at first incredibly scary soon became our normal mealtime routine. She needed to be held upright to eat and for some time afterward due to the reflux, so this became her naptime. I don’t know if this was partly the cause of her incredible cuddly nature, but other moms would marvel at the fact that she loved being held when their own babies would squiggle away from them. Meanwhile I would both marvel and grieve at how they fed their babies so effortlessly. I kept Holli in a co-sleeper by my bed until she was a year old, and used an Angel Care monitor, which would supposedly alarm me if she were to stop breathing, until she was almost 3. After all of the monitoring in the NICU it was tough to not have any, so this gave me some peace of mind. To this day, I still check to make sure she is breathing when I go in to say goodnight after she falls asleep.
Because she could not breastfeed I pumped for hours, and mixed this breast milk with formula as instructed, for extra calories. More often than not, this “liquid gold” would end up all over me or the sofa due to either a tube malfunction or her reflux. This terrible reflux got her awarded with the (distinction) “failure to thrive.” Although I worked hard to avoid it, when Holli was 6 months old she underwent surgery have her feeding tube enter directly into her stomach. Thankfully she started to thrive.

I now know that many thought I was naïve. What sometimes seemed a relentless and incredibly frightening stream of bad news, I always believed she would be just fine. I could not think otherwise; there was no other option but that she would be okay. And she defied the odds, every time. I also now know how incredibly lucky we are, and how many babies and parents are not so lucky. This both frightens me and humbles me incredibly.
Holli was followed by a host of professional providers until her second birthday to monitor her progress. Babies who do not have the full amount of time to grow in the womb do not have the flexion skills that develop as a result of being enfolded in a small space and pushing to get out. I was told that by two years she should catch up to her peers. She more than did so verbally, causing everyone she encountered to wonder at this tiny 2-year old girl who spoke with the vocabulary of a four year old but could pass for a one-year old. Physically, however, she lagged behind. She was slow to roll over, never crawled but instead “bum-scooted,” and waited until she was 20 months old to suddenly walk as though she’d been doing it forever. I read at one point that babies concentrate on one thing at a time, and believe that she concentrated wholeheartedly on talking as much as she could (and still does!) while putting off the inevitable need to venture out physically. This was actually a blessing in disguise as just 2 weeks after she started walking, my twins were born. I’m not sure how I would have run after her on the playground, as large and as nauseated as I was, were she as active as her peers.

Today Holli is almost 5 years old and my twins are 3. Each time we go out, people ask if I have triplets. Although still tiny, she is increasingly less hesitant about physical obstacles, and seemingly has no idea of her stature when it comes to asserting herself. Often the phrase “Napoleon complex” comes to mind as I watch her. She is the first to raise her hand and speak up in a crowd, and is still as cuddly and sweet with not only her family and friends, but those she is meeting for the first time. She instructs her younger brother and sister in the roles they will play in her imaginative games, and they believe she walks on water. She still speaks and thinks like a much older child, astounding me constantly with her thought processes. I sometimes wonder if the strength she needed to survive early on forced this strength, determination and uncommon intelligence for her age, or if this would have been her nature regardless. What I do know is that as difficult and sometimes heartbreaking as it was, her inauspicious beginnings did not break her spirit, or mine.
All content on this Web site, including medical opinion and any other health-related information, is for informational purposes only and should not be considered to be a specific diagnosis or treatment plan for any individual situation. Use of this site and the information contained herein does not create a doctor-patient relationship. Always seek the direct advice of your own doctor in connection with any questions or issues you may have regarding your own health or the health of others.

Cait James is a single mom by choice to a singleton and twins who recently moved her family, grandma and all, from California to the Pacific Northwest. She is enjoying exploring the forests and beaches in her new surroundings with her children, and watching the wonder in their eyes. She has spent her career in pediatric and adult nutrition, and now takes a special interest in clients with feeding tubes due to her experience with her singleton. Eventually she will get back to being a morning runner, but for now she revels in her time with her fellow early bird little people… and then piles the crew in the car and heads outside or to the gym!
Related Articles
- Formula Fed to Breastfed: Transitioning After The NICU
- What Are The Different Levels of NICU?
- Twins In The NICU: Our 80 Day Journey Home
Expecting Twins?
START HERE!
Check out our ultimate list of the most important articles for expecting twins
and managing your newborns!
Are You a New Twin Parent?
Check out Natalie Diaz’s book:
“What To Do When You’re Having Two
The Twin Survival Guide From Pregnancy Through the First Year”
In What to Do When You’re Having Two: The Twins Survival Guide from Pregnancy Through the First Year, national twins guru and founder of Twiniversity (and twin mom herself!) Natalie Diaz provides a no-holds-barred resource about life with twins, from pregnancy and birth all the way through your duo’s first year of life.
Accessible and informative, What to Do When You’re Having Two
is the must-have manual for all parents of twins.
Have you taken your expecting twins class yet? We offer a great class on demand so you can take it on your own schedule! There are so many video modules covering everything from your twins’ baby registry to your first week at home with twins! Sign up today to get started before your twins arrive.
Need some twin parent friends? Get the support you need with a Twiniversity Membership. Benefits include a monthly twin parent club meeting on Zoom, access to a private Facebook group just for twin parents, and a video library of twin parenting lessons. Visit Twiniversity.com/membership to join today!

Twiniversity is the #1 source for parents of
multiples, and we are growing faster every day!
Find us all over the web:
Or contact us by email at community@twiniversity.com










