Last updated on February 5th, 2024 at 04:40 pm
You may have heard these long words talked about by your pediatrician – Torticollis (tore-ti-call-us) and Plagiocephaly (play-jee-oh-sef-uh-lee) – but what do they mean? Or have you seen a baby wearing a helmet and wondered why?
These diagnoses have exploded over the past 20 years. Initially, the Back to Sleep program of 1992 was blamed, but new research is showing that all of our baby “containers” (car seats, swings, etc) are also playing a role in the increased incidence.
The term torticollis is derived from the Latin terms “tortus” (meaning twisting) and “collum” (meaning neck). In simple terms, torticollis refers to any asymmetrical positioning of the head or head tilting. Alarmingly, torticollis affects 57% of twins! But don’t be concerned, torticollis is easily corrected and typically has no long-term effects when identified and treated early. Most pediatricians are screening for torticollis as early as the 2 month well child appointment.

The term plagiocephaly refers to any abnormal shape of the head; it is often referred to as “flat head syndrome”. Nearly 47% of babies have some form of plagiocephaly, but only 10% of those need treatment with a cranial remolding orthosis or “helmet”. Plagiocephaly is present in 90% of babies with torticollis; while we don’t know which comes first (the chicken – torticollis – or the egg – plagiocephaly), we do know that because of this strong association it is important to be aware of both.
Torticollis can be either congenital (present at birth) or acquired (develops after birth). Congenital torticollis is resultant from in utero positioning or crowding due to large birth size or multiple fetuses; this is why the incidence is so high in twins.
Treatment for congenital torticollis should begin immediately following birth. Acquired torticollis is resultant from persistent positioning of the head or neck in one position; treatment should begin as soon as any type of positional preference is observed – the earlier the better.
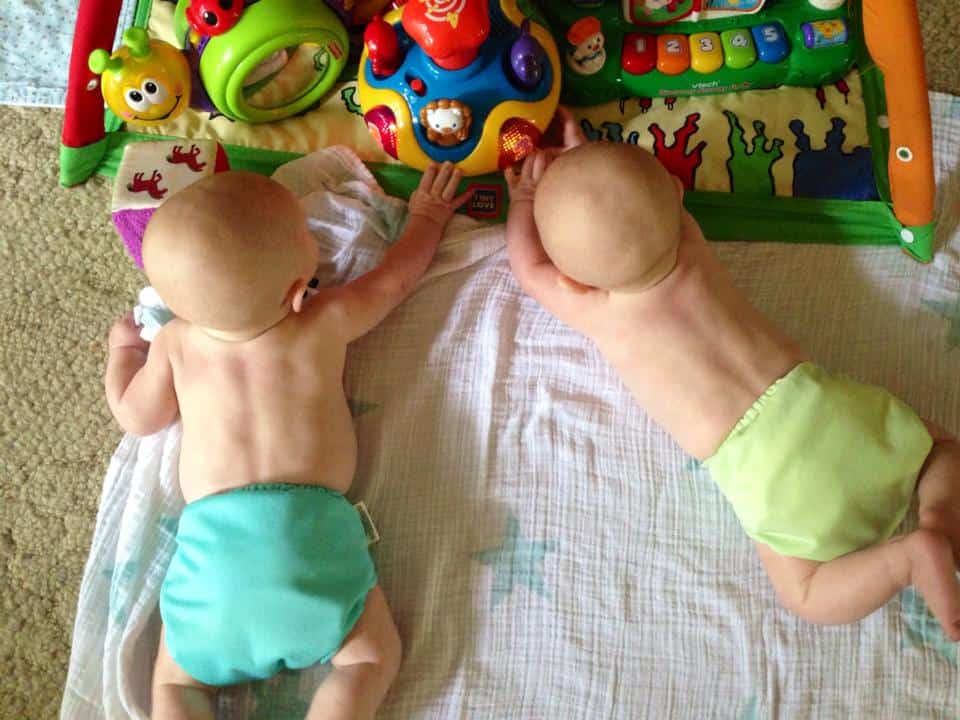
Plagiocephaly can also develop from in utero positioning and is also much more common with multiple births. Babies’ skulls are incredibly soft and malleable; plagiocephaly can develop in as little as one week with persistent positioning on one part of the skull (premature babies are at even higher risk).
It is important to adopt the “back to sleep, tummy to play” recommendation, as well as to limit time in infant carriers and positioning devices. In the early days when your baby may be sleeping a lot and not tolerating a lot of tummy time when awake, side-lying positioning for play and baby wearing are extremely effective ways to limit pressure on the back of the skull.
There are two main strategies for prevention and treatment of torticollis and plagiocephaly: 1) supervised tummy time 2) repositioning techniques. When your baby is awake, the more tummy time the better – the skull is completely free of pressure in this position, the muscles of both sides of the neck are activated to lift the head, and baby is building core muscle strength that will help with posture, breathing, and digestion.

Use a variety of positions with your baby during play – tummy, back, left side, right side, and supported sitting. If your baby is showing a preference to turn his head one direction, position yourself or objects of interest (toys, mirrors, etc) on his non-preferred side. If your baby isn’t showing a preference – rotate!
If your baby is diagnosed with torticollis and/or plagiocephaly do not despair! First of all, you are not alone. Second, the earlier these are identified the shorter the treatment time; babies with torticollis should begin physical therapy treatment between 2 and 4 months of age and babies with plagiocephaly should begin treatment between 4 and 6 months of age. Repositioning alone for treatment of plagiocephaly is most effective prior to 4 months of age.
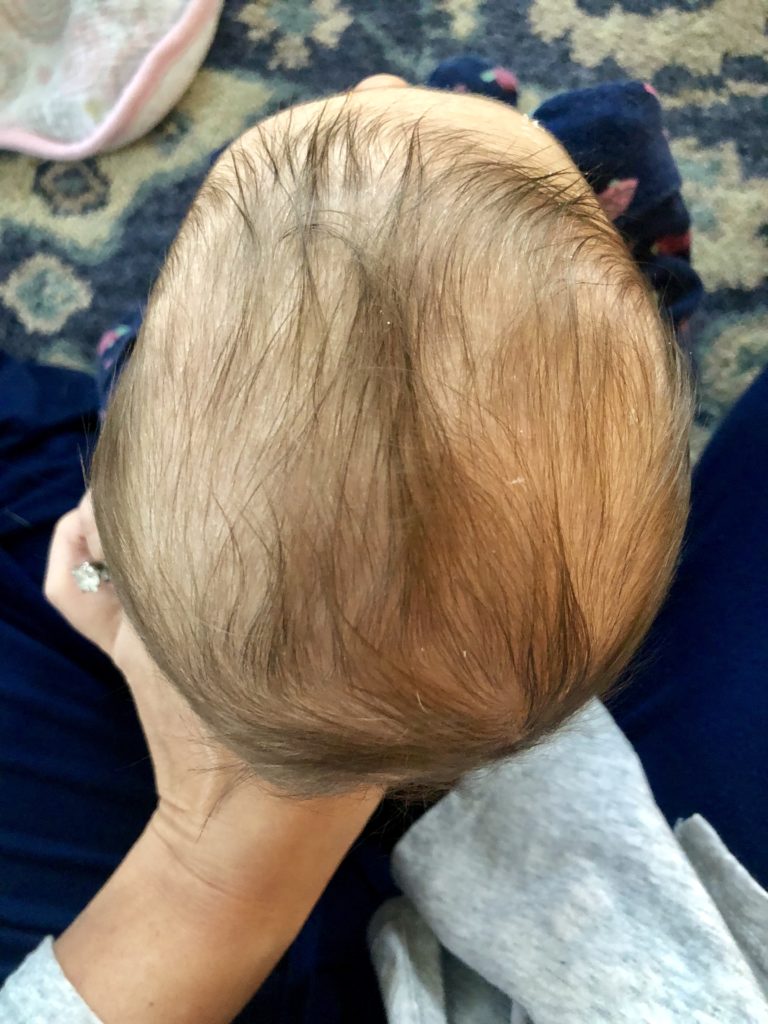
A common question that arises is “Isn’t plagiocephaly just cosmetic? I think my baby is beautiful even if his head isn’t perfectly round.” While much research has shown that plagiocephaly has NO effect on brain development, there are some long term effects if left untreated:
- Standard safety helmets (bike helmets, sports helmets) will not fit properly on an asymmetrically shaped head and could put your child at risk for injury.
- Because the jaw is attached to the skull, asymmetries may affect the jaw position and result in a crossbite or overbite.
- If facial asymmetries are present, eyeglasses may not fit properly.

You can do a quick screening at home to determine if your baby may have torticollis and/or plagiocephaly.
- Place your baby on his back and have him track your face or an object – is he able to turn his head to both sides equally?
- Look back at pictures you have taken of your baby – is his head always tilted or turned to one side?
- Place your child in a supported sitting position and look at him top down – does one side of the forehead seem more forward? Does the back of the head look flat on one or both sides? Does one ear appear to be more forward?
- Look at baby’s face – does one eye appear smaller or one cheek appear fuller?
If you answer yes to any of these questions, the first step would be to discuss your concerns with your pediatrician. Early intervention and physical therapy are services available to address torticollis. Additionally, many orthotics companies offer free plagiocephaly screenings with a referral from your pediatrician. Remember, it is never too early to take action!

Stacey Haught is a mom to 7 year old Madison, 6 year old twin boys – Mason and Mitchell, and 18 month old twin girls – Sadie and Sophia. She is a pediatric physical therapist but has put her career on hold to stay at home with her rambunctious 5 kids. She resides with her husband and kids just outside of Pittsburgh, PA. Her family enjoys everything outdoors regardless of the season – finding new sledding hills, exploring area parks, and hiking and camping at their family cabin.
References for Torticollis/Plagiocephaly
- De Chalain, Tristan M., et al. “Torticollis Associated with Positional Plagiocephaly: A Growing Epidemic. The Journal of Craniofacial Surgery. May 2005.
- Graham, John M., et al. “Management of Deformational Plagiocephaly: Repositioning Versus Orthotic Therapy.” The Journal of Pediatrics. February 2005.
- Hollier, Larry M.D., et al. “Congenital Muscular Torticollis and the Associated Craniofacial Changes.” Plastic and Reconstructive Surgery. March 2000.
- Kaplan, Sandra L., et al. “Physical Therapy Management of Congenital Muscular Torticollis: An Evidence-Based Clinical Practice Guideline.” Pediatric Physical Therapy. January 2013.
- Littlefield, Timothy R, et al. “Multiple-Birth Infants at Higher Risk for Development of Deformational Plagiocephaly: Is One Twin at Greater Risk?” Pediatrics. January 2002.
- Rogers, Gary F., et al. “The Role of Congenital Muscular Torticollis in the Development of Deformational Plagiocephaly.” Plastic and Reconstructive Surgery. February 2009.
- Stellwagen, L., et al. “Torticollis, Facial Asymmetry and Plagiocephaly in Normal Newborns. Archives of Disease in Childhood. 2007.
- Van Vlimmeren L.A., et al. “Torticollis and Plagiocephaly in Infancy: Therapeutic Strategies.” Pediatric Rehabilitation. 2006.
Related Articles – Identifying and Managing Plagiocephaly and Torticollis in Infants
- What is Tummy Time and Why Should I Do It?
- Torticollis: A Physical Therapist’s Perspective
- So Your Baby Might Need a Helmet
- How Can I Avoid Flat Head Syndrome?








