You are so close to the finish line! You may be feeling really uncomfortable now, which is to be expected when you’re 35 weeks pregnant with twins. Hang in there!
What can you expect at 35 weeks pregnant with twins? We’ve compiled a list of common symptoms, to-do’s this week, pregnancy tips, pregnancy concerns, questions to ask your doctor, advice from other pregnant moms of twins, and tons of other info below to help you through this week in your twin pregnancy. Enjoy!
Facebook | Instagram | YouTube | Twitter | Pinterest
⬅ 34 Weeks Pregnant with Twins 👶👶
👶👶 36 Weeks Pregnant with Twins ➡
- 35 Weeks Pregnant Video
- What’s Going On With Those Twinnies?
- To-Do List
- 5 Tips for a Better 35th Week
- Advice From Other Twin Moms
- Questions Twin Moms Had for Their Doctor
- Typical Tests That Are Done
- Product Recommendations
- An excerpt from “What To Do When You’re Having Two”
- Belly Photos at 35 Weeks Pregnant With Twins
- Ultrasound Photos at 35 Weeks Pregnant With Twins
- Articles You Should Read This Week
- Videos to Check Out
- Register for Class
35 Weeks Pregnant Video

Our new digital twin pregnancy journal is up for sale on the Twiniversity Etsy store! This is the first and only digital journal exclusively for twin pregnancy. It’s the perfect way to record your precious twin pregnancy memories to cherish for years to come. Click here to learn more… and while you’re at it, check out our expecting twins classes and Twiniversity Shop!

What’s Going On With Those Twinnies?
- Median weight for dichorionic twins: 5lbs, 7oz
- Median weight for monochorionic twins: 5lbs, 4oz
Your twins’ kidneys are now fully developed, and their livers can process some waste products.
To-Do List
- Rest. Rest. Rest. If you’ve made it this far, do all you can to make it even further. And by that, we mean do pretty much nothing. Lay down whenever you can. Watch all the Netflix shows you’ve been meaning to get to. Keep those babies cooking as long as you can.
- Work on a pregnancy scrapbook to pass the time. If you’re a crafty person, get into it with hands-on materials, glue, and all the glitter you can handle. If you’re not crafty, pull up your laptop and let a photo book website do the work for you.


5 Tips for a Better 35th Week
- Have your bags packed and ready to go.
- Eat slowly to avoid indigestion.
- Stay off your feet as much as possible.
- Get things done before lunch because after lunch is just plain exhausting.
- The more pillows, the better!

Advice From Other Twin Moms
Hang in there! So close to the end. Rotate between sitting with feet up and walking around. If you’re uncomfortable, move.
– Meredith, Texas
Relax and take it day by day. It’s great that you’ve made it this far!
– Brooke A., Osteen, FL
Slow and steady will win the race. We’re only human and growing two babies is not an easy task. Go easy on yourself.
– Farrah M.
Get takeout or have someone cook for you. Lay down a lot.
– Stephanie G., Petaluma, CA
It’s a temporary state of utter discomfort. Accept the help from others. Don’t beat yourself up for resting.
– Lynn F., Wrentham, MA
Take it easy and listen to your body. It’s amazing that you’ve made it this far and even though at this point you’re probably so over being pregnant it’s what is best for your babies and each day they stay in lessens the chance of NICU stay.
– Jessica C., San Marcos, CA
Need some twin parent friends? Get the support you need with a Twiniversity Membership. Benefits include a monthly twin parent club meeting on Zoom, access to a private Facebook group just for twin parents, and a video library of twin parenting lessons. Visit Twiniversity.com/membership to join today!

Concerns Other Twin Moms Had
Anxiety about giving birth.
Will I need to be induced?
Do I have everything ready?
Is my sleeping set up ok?
Can we all avoid the flu?
Will I be able to lose weight after the birth?
Is there anything else I need to do before babies come?

Questions Twin Moms Had for Their Doctor
Are the twins measuring the same?
Should I plan for a c-section or vaginal birth?
This is the week they do the MRSA and strep B swab for c-section recipients and I’m interested in those results.
What is the plan if I don’t go into labor naturally?
Does the hospital provide a belly binder? And is this recommended?
Does the hospital have a policy for visitors since it’s flu season?
Is there anything I should be watching regarding swelling?
Is baby A still head down?
What are other ways to induce labor that don’t involve drugs?
What can I expect before, during, after the c-section?
Is my husband able to cut the umbilical cords during a planned c-section?
When should I go to the hospital once contractions start?
Typical Tests That Are Done
It is common to have weekly nonstress testing (NST) with fluid assessments starting at 32 weeks in an uncomplicated twin gestation. As your pregnancy progresses you will likely be scheduled more and more frequently, building to every 1-2 days as you get closer to full term. A nonstress test is used to evaluate your babies’ health before birth. The goal of a nonstress test is to provide useful information about your babies’ oxygen supply by checking their heart rates and how it responds to your babies’ movements. The test might indicate the need for further monitoring, testing, treatment or delivery. A nonstress test typically requires no special preparation. During the nonstress test, you’ll lie on a reclining chair. You’ll have your blood pressure taken at regular intervals during the test and each baby will be monitored while you relax in a recliner for 20 minutes, playing on your phone or reading a book.
A fetal biophysical profile (BPP) is a prenatal test used to check on a baby’s well-being. The test combines fetal heart rate monitoring (nonstress test) and fetal ultrasound to evaluate a baby’s heart rate, breathing, movements, muscle tone, and amniotic fluid level.
The Centers for Disease Control and Prevention (CDC) has recommended routine screening for vaginal strep B for all pregnant women. This screening is performed between the 35th and 37th week of pregnancy. Studies show that testing done within 5 weeks of delivery is the most accurate at predicting the GBS status at birth. Group B streptococcus (GBS) is a type of bacterial infection that can be found in a pregnant woman’s vagina or rectum. This bacteria is normally found in the vagina and/or rectum of about 25% of all healthy, adult women. Women who test positive for GBS are said to be colonized. A mother can pass GBS to her baby during delivery. GBS affects about 1 in every 2,000 babies in the United States. Not every baby who is born to a mother who tests positive for GBS will become ill. Although GBS is rare in pregnant women, the outcome can be severe. As such, physicians include testing as a routine part of prenatal care.
If you are having a c-section you may be tested for MRSA. MRSA stands for methicillin-resistant Staphylococcus aureus. It is a type of staph infection. Even if a pregnant woman contracts MRSA in her pregnancy, it’s easy to treat. Antibiotics will cure most cases, and they’re safe for a developing baby to be exposed to. A baby will only get the infection if he comes into contact with it through vaginal delivery. Many women must be screened for MRSA when they need a C-section because hospitals must screen every surgery patient for the infection prior to the operation. To perform the screening, a nasal swab is collected by rotating a swab inside each nostril. Occasionally, a swab of a wound infection site or skin lesion is collected.

Product Recommendations
Best Cradle – Maternity Support Belt
Palmer’s Cocoa Butter Tummy Butter & Stretch Mark Massage Lotion
Rachel’s Remedy Breastfeeding/Sore Breast Relief Packs
Digital Twin Pregnancy Journal
Boppy Pregnancy Support Pillow
Check out this list of more Must Have Pregnancy Products You Need Right Now and Postpartum recovery products that twin moms LOVE
Check out all our Twiniversity merch in our SHOP! We’ve got twin mom and dad t-shirts, twin planning printables, lactation support, twin baby shower planners & games, a digital twin pregnancy journal, and so much more! Start shopping now


An excerpt from “What To Do When You’re Having Two“
If you are being induced, your pre-delivery experience will be very similar to that of a C-section. If you are home and you go into labor naturally, that’s a different story. You should be prepared for your delivery anytime after your 34th week. There is a very good chance you’ll go beyond that time, but your uterus will be pretty large by then and labor could kick in sooner than expected.
If you’re home and you start feeling contractions, grab a stopwatch and see how far apart they are. If you are having four or more contractions or even eight in an hour, call your doctor and give him a heads up. For new parents, you don’t want to rush too much because the labor process could take quite some time, but you don’t want to drag your heels, either. Usually, after you’ve entered active labor, you still have between 8-12 hours before the babies will be born. If you are home and your water breaks, immediately call your doctor and head over to the hospital. Your doctor will want to check for any sign of infection because the babies are no longer protected by the amniotic sac.
Pregnant with twins and not sure where to start? Visit the Ultimate Twin Pregnancy Guide to find all the top articles and resources to get you ready for twins. While you’re at it, check out our expecting twin classes and Twiniversity shop!
REMINDER: Don’t forget to take a belly shot!
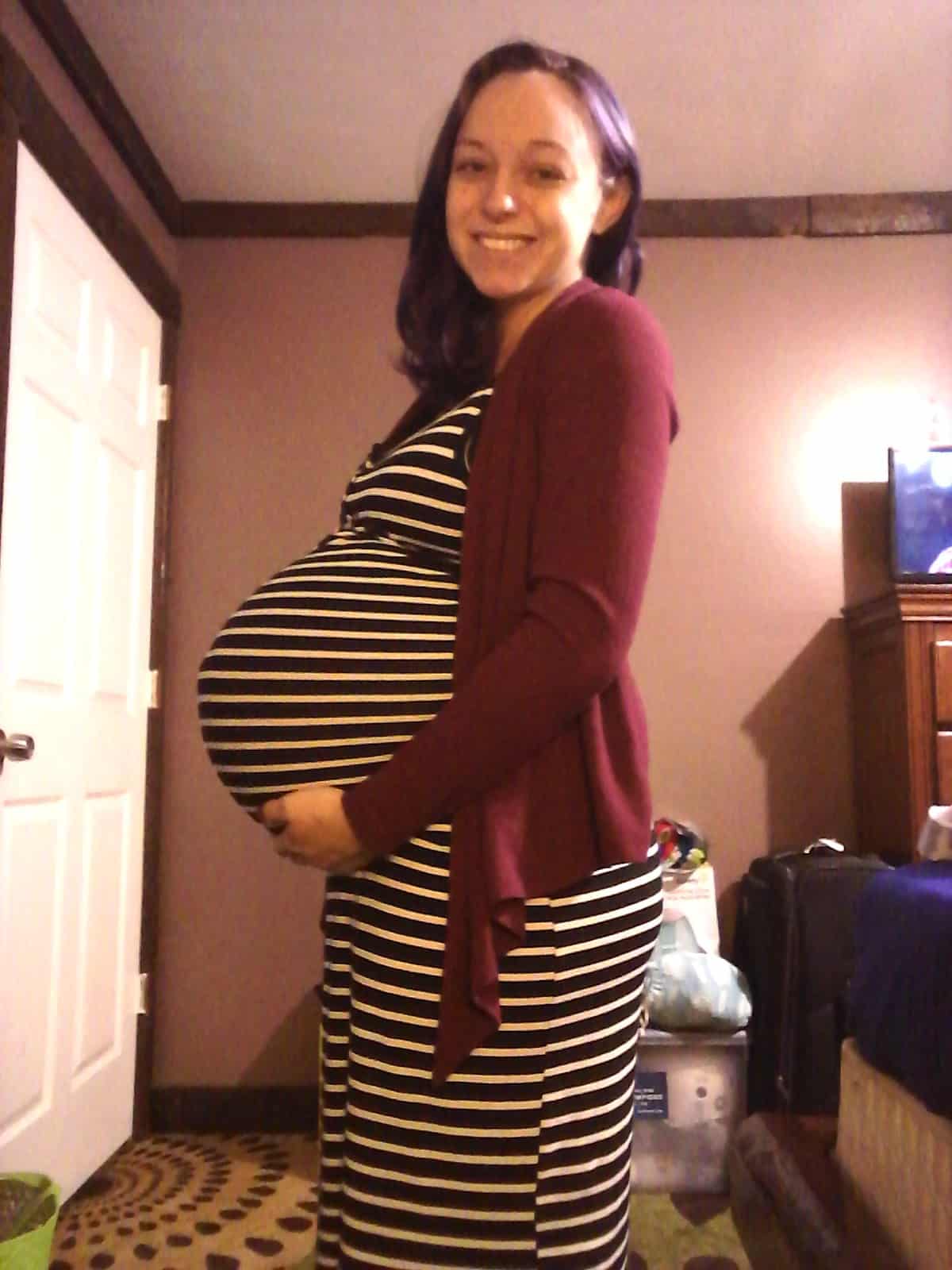
Belly Photos at 35 Weeks Pregnant With Twins

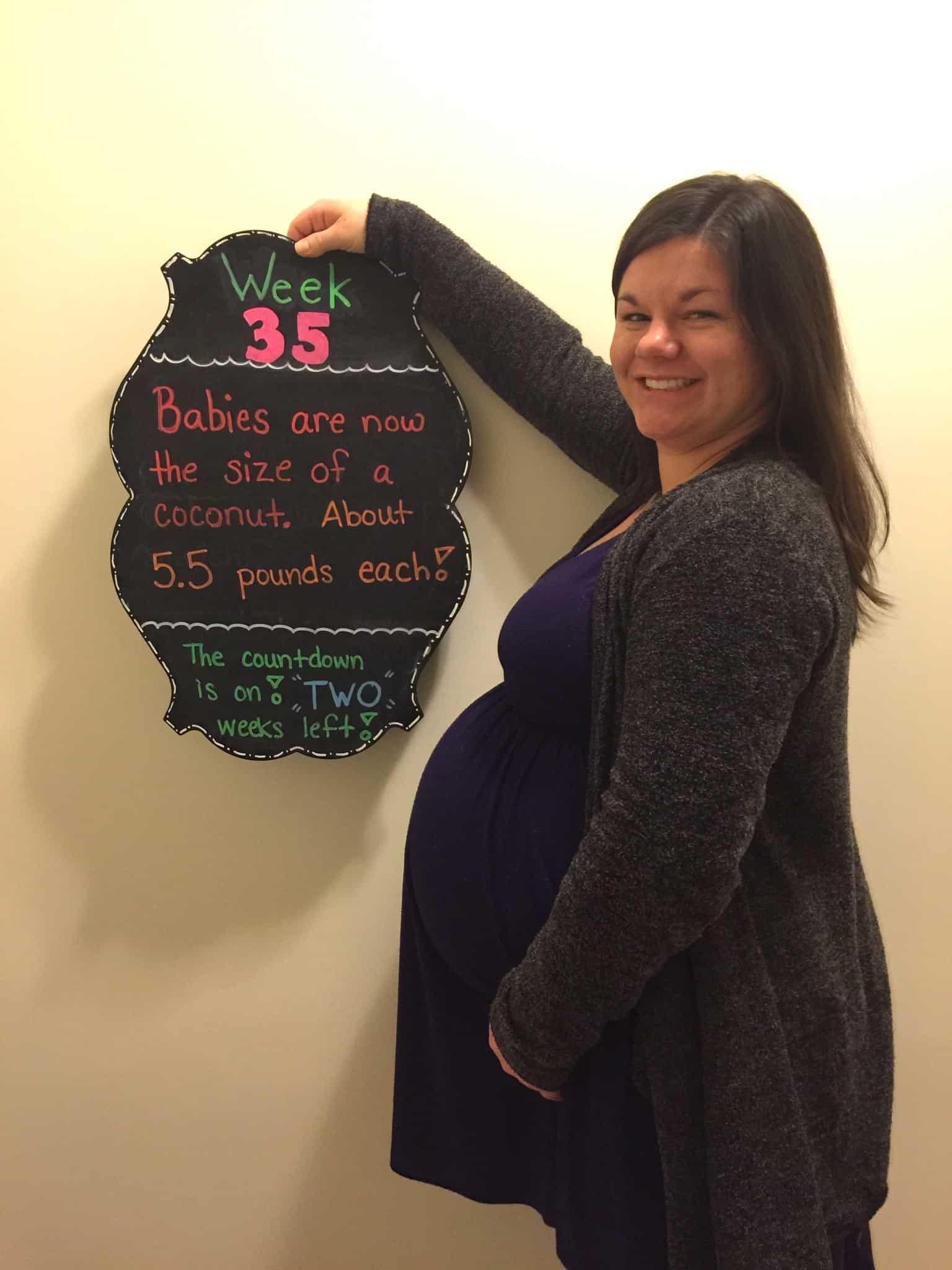

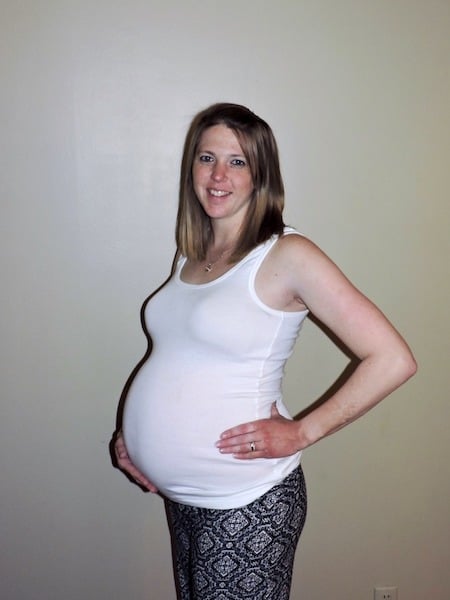
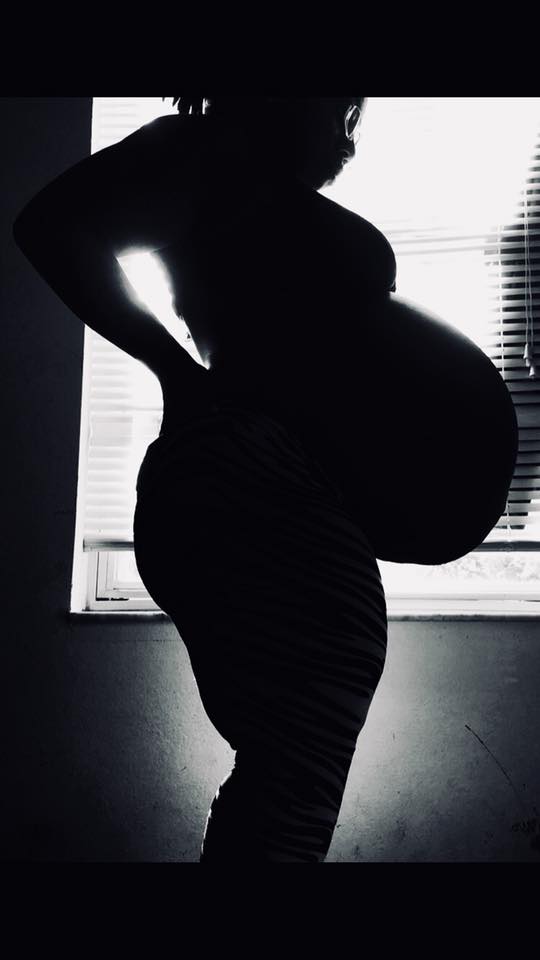


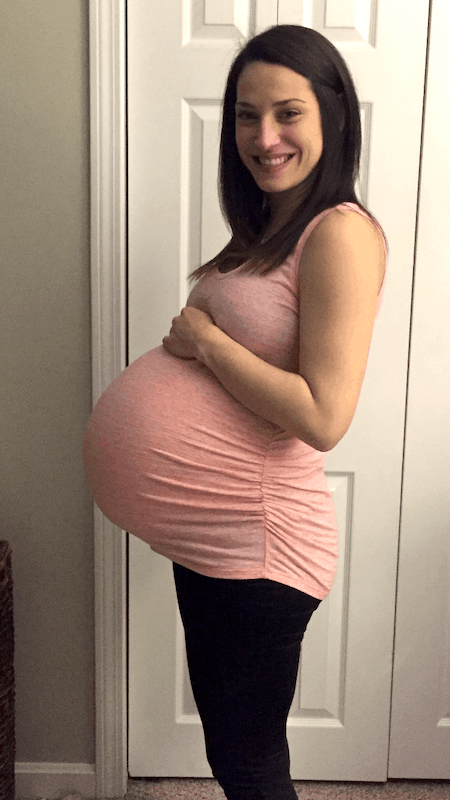
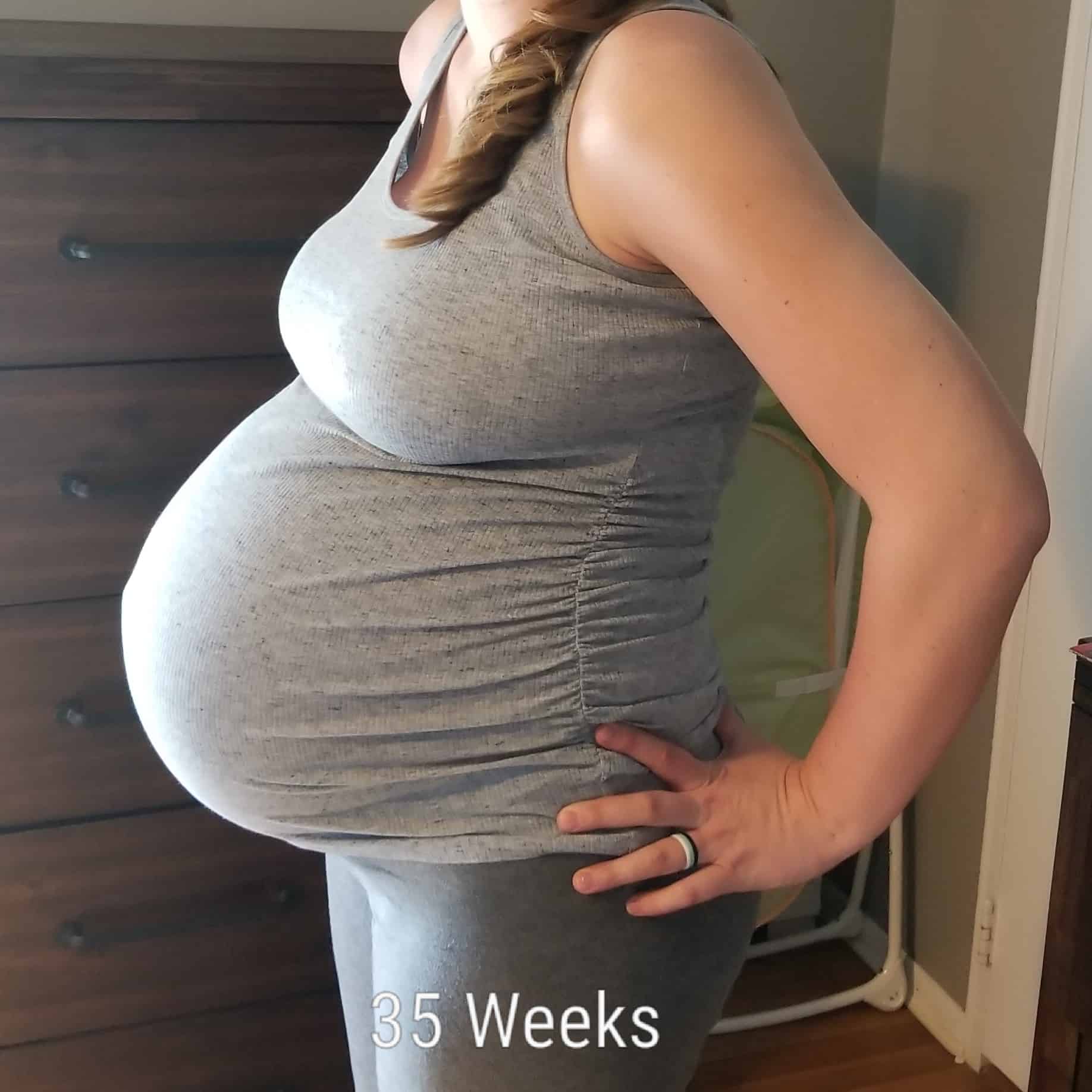


Ultrasound Photos at 35 Weeks Pregnant With Twins
Articles You Should Read This Week
My Emergency C-section Delivery with Twins
When Nothing Goes to Plan: My Double-Whammy Twin Birth
Finding the Strength to Accept a C-Section
Videos to Check Out
Register for Class
Have you taken your expecting twins class yet? We offer a great class on demand so you can take it on your own schedule! There are so many video modules covering everything from your twins’ baby registry to your first week at home with twins! Sign up today to get started before your twins arrive.
Need a plan for the first week home with twins? Book your 60-minute twins \post-delivery strategy session on a video call with Lauren Oak, Twin Expert and Certified Postpartum Doula (and mom of twins!), to create a customized game plan for you and your twins when they come home. Click here to learn more… and while you’re at it, check out our Twiniversity Shop and Twin Parent Memberships.

Want to get weekly emails about your twin pregnancy? Sign up for the Twiniversity email list! Subscribe today to get emails about giveaways, events, weekly article roundups, and more! We’ll be sending you a weekly twin pregnancy email to keep you on track with your pregnancy to-do list! Click here to learn more… and while you’re at it, check out our expecting twins classes and personal twin parent coaching services.
⬅ 34 Weeks Pregnant with Twins 👶👶
👶👶 36 Weeks Pregnant with Twins ➡
Sources
- AAFP. 2011c. Your baby’s development: The third trimester. American Academy of Family Physicians.
- Mayo Clinic. 2014b. Fetal development: The third trimester.
- MedlinePlus (ADAM). 2015. Fetal development.
- OWH. 2010. Stages of pregnancy. U.S. Office on Women’s Health.
- ACOG. 2015. FAQ156. Prenatal development: How your baby grows during pregnancy. American College of Obstetricians and Gynecologists.